Gut Health Basics: Digestive System – the Body’s Core Engine
Digestive symptoms can feel unpredictable because digestion isn’t controlled by food alone. It’s influenced by your nervous system, immune system, hormones, and even your overall stress “state.”
This is why two people can eat the same meal and have completely different outcomes. It’s also why you can do an elimination diet “perfectly” and still feel off, because the digestive system is not a simple machine. It’s a living system that responds to your internal and extrenal environment.

In this article, I’ll explain digestion in simple everyday words, and then I’ll show you how everything connects and influences your health and wellness using my 3-layer framework: Body, Mind, Energy. This perspective is shaped by my own experience and the patterns I’ve seen in the people I’ve worked with. It’s for education and insight, not personalized medical advice.
Digestion has 5 jobs
Think of your digestive system as a long processing line with five main jobs:
- Break food down into usable pieces
- Absorb nutrients into the body
- Protect you (keep threats out while letting nutrients in)
- Move things along at the right speed
- Eliminate waste comfortably and consistently
When digestion feels “off,” it usually means one (or more) of these jobs isn’t running smoothly. That’s it. Just a system that’s overloaded somewhere.

A quick tour of digestion
Mouth: the prep kitchen
Digestion starts before you even swallow. Chewing is like chopping ingredients before cooking. The better you chew, the easier everything downstream becomes. Your saliva isn’t just moisture. It softens food, helps it slide down smoothly, and contains enzymes that start breaking down carbohydrates. Even smelling and tasting food signals your body to “turn digestion on,” preparing the stomach and intestines for what’s coming.
Esophagus: the conveyor belt
Your esophagus moves food to the stomach with wave-like squeezes (like a toothpaste tube). It’s not supposed to burn, feel tight, or feel like food is getting stuck.
When this step is disrupted:
Reflux, irritation, or poor timing between the stomach and esophagus can create heartburn, regurgitation, or that “lump in the throat” feeling. Some people also notice symptoms when eating too fast or lying down soon after meals.
Stomach: the acid blender
Your stomach churns food and mixes it with acid. This helps break down protein, supports mineral release, and acts as a first “filter” against microbes. The stomach also releases food into the small intestine in a controlled way: too fast or too slow can trigger symptoms.
When this step is disrupted:
- Low stomach acid or weak churning can mean protein-heavy meals feel hard to digest, with heaviness, nausea, or more gas later.
- Poor timing of stomach emptying can contribute to reflux, bloating, or feeling full quickly.
- Irritated stomach lining can make the upper gut feel sensitive even with small meals.
(Note: people can have reflux even with low acid—reflux is often about pressure/timing, not just “too much acid.”)
Small intestine: the nutrient extraction zone
This is where most nutrient absorption happens. It gets support from:
- the pancreas, which releases digestive enzymes (scissors for protein, fat, carbs)
- liver + gallbladder add bile (like dish soap) to break fat into tiny droplets so enzymes can work.
- the small intestine lining is covered in millions of tiny folds (villi/microvilli). Picture a thick, fluffy carpet, designed to maximize surface area so you can absorb nutrients efficiently.
The gut lining: the security gate
This is one of the most important parts of digestion, and it’s also where a lot of modern gut issues live.
Your gut lining has:
- A mucus layer (like a thin protective gel coating)
- Tight junctions between cells (like zipper teeth sealing the gaps)
- Immune cells nearby (like security guards)
- Beneficial microbes that help maintain order (like helpful staff)
This barrier is essential: it decides what gets into the body and what stays in the gut.
When this step is disrupted:
If the lining is inflamed or the “zipper” isn’t regulating well, you develop a “leaky gut” allowing bacteria, toxins, and undigested food particles to pass into the bloodstream. Then your immune system may get more reactive. This can look like increasing sensitivities, unpredictable reactions, or inflammatory symptoms that linger beyond one meal.
Large intestine (colon): Microbial composting + water-recycling center
- Absorbs water and electrolytes.
- Gut microbes ferment leftover fibers and produce helpful compounds (like short-chain fatty acids) that support the colon lining and immune balance.
- Forms and stores stool for exit.
When this step is disrupted:
- If motility (movement of food that your nervous system and hormones coordinate) is too slow, stool sits longer, then this leads to constipation, bloating, heaviness and more fermentation gas.
- If motility is too fast, less water is absorbed, resulting in looser stools, urgency, diarrhea, cramping, less absorption time.
- If the microbial balance is off (too few beneficial strains, and/or too many opportunistic microbes) certain foods can create excessive gas, discomfort, or irregular stool patterns.
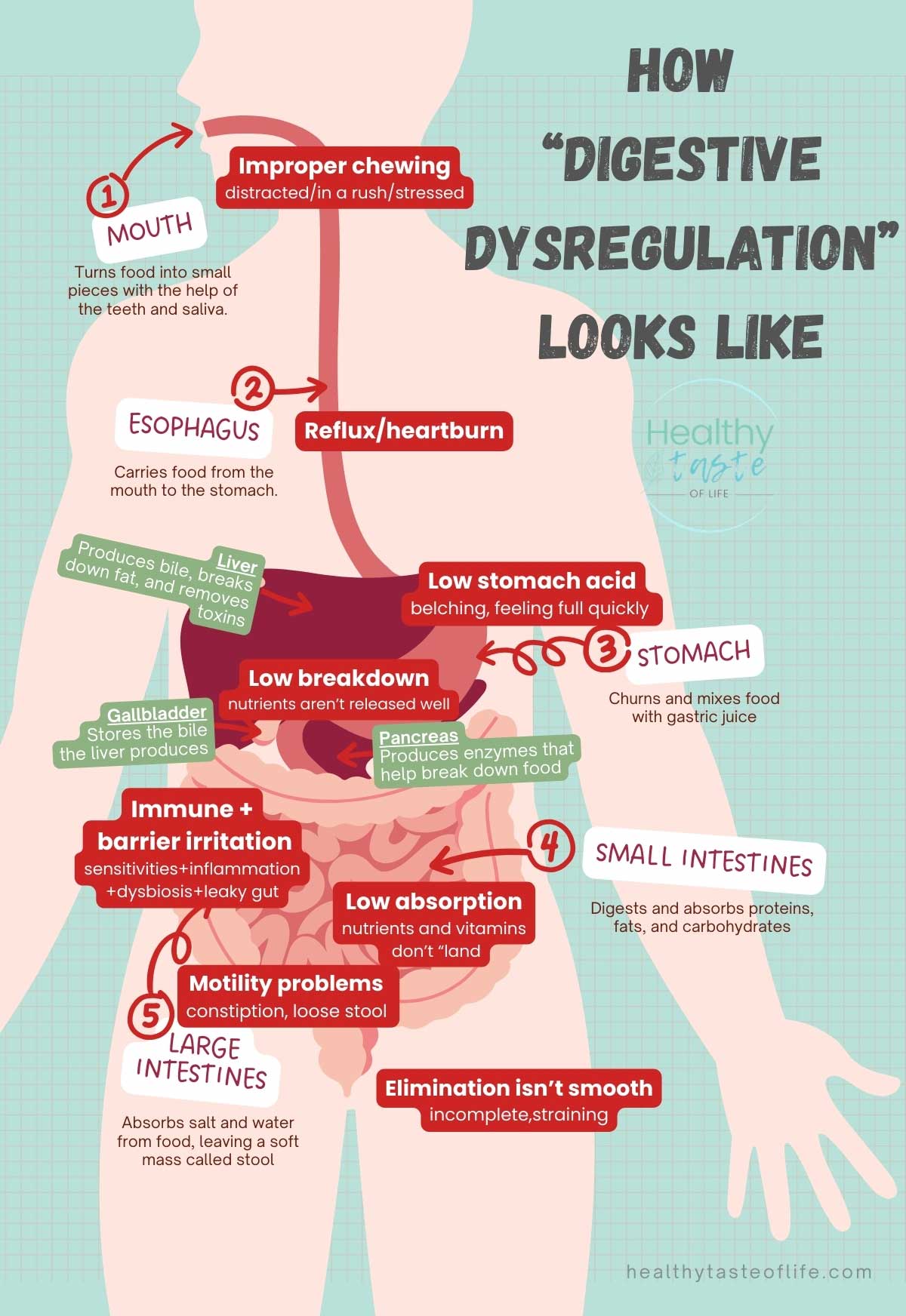
What “digestive dysregulation” actually means (The 5 Jobs)
Let’s translate “dysregulation” into normal language. Usually it means one or more of these:
1) Low breakdown (the “prep work” doesn’t keep up)
This can look like:
- heaviness after meals
- reflux/burping
- nausea after eating
- feeling full quickly
- sometimes greasy or floating stools (fat digestion signs)
Common reasons low breakdown happens:
- Eating too fast / not chewing enough (big pieces are harder to process)
- Stress while eating (fight-or-flight lowers digestive secretions and coordination)
- Low stomach acid output or weak stomach “churning”
- Low enzyme output from the pancreas (food isn’t fully split into absorbable parts and you get sensitivity to certain food /chemicals)
- Low bile flow (fats feel heavy; more greasy stool patterns)
- Irregular eating (grazing all day, snacking, late-night eating) digestion never gets a clear rhythm
- Highly processed diet patterns + low micronutrients.
- Certain meds can affect digestion for some people (varies by person)
2) Low absorption (low assimilation)
You can be eating “well” and still feel depleted if absorption is impaired. If your gut lining is irritated, inflamed, or moving too fast, “breakdown” is weak – nutrients aren’t released well. It’s like having groceries delivered to your porch but not being able to bring them into the house.
This can look like:
- Low energy + brain fog + weakness (crashing easily) even though you’re eating “healthy”.
- Muscle cramps, twitchiness, restless legs (can be linked with magnesium/electrolyte patterns)
- Nutrient deficiencies (iron, B12, vitamin D, etc.)
- Tingling/numbness in hands/feet, shaky feeling (sometimes linked with B vitamin patterns)
- Dizziness, shortness of breath with exertion, paleness (often linked with low iron patterns)
- Loose stools/urgency (food moves too fast to absorb well)
- Greasy, bulky, or hard-to-clean stools (a clue fats aren’t being absorbed well for some people)
- Subtle “depletion” signs over time like hair shedding, brittle nails, dry skin, slower wound healing or getting cold easily.
- Unexplained weight and appetite changes (trouble maintaining weight despite eating enough or feeling hungry again quickly because meals don’t “land”).
3) A jumpy security gate (immune + barrier irritation)
This can look like:
- Increasing food sensitivities (more foods start to bother you)
- Reactions that aren’t consistent (a food is fine sometimes, not fine later)
- Symptoms that linger beyond one meal (you feel “inflamed” for a day or more)
- Bloating + discomfort that feels more like irritation than simple fullness
- Stool changes that come and go (looser, mucus for some people)
- Sometimes systemic spillover: chronic fatigue, brain fog, skin rashes and dryness, achy joints, muscle weakness during gut flares.
What can cause it (common drivers):
- Ongoing irritation in the gut (from infections, food poisoning history, mold, chronic reflux/irritants, alcohol, or very processed foods for some people).
- Chronic stress / poor sleep (keeps the nervous system in threat mode, which can weaken barrier regulation over time).
- Inflammation from immune conditions (like IBD, celiac, Thyroiditis (thyroid) autoimmune patterns).
- Medication impacts (especially frequent NSAID use like ibuprofen; antibiotics can shift microbes).
- Microbial imbalance (dysbiosis) (less protective microbes, more bad ones, more fermentation in the wrong place).
- Nutrient depletion (your lining renews fast; low protein, zinc, vitamin A, etc. can make repair harder).
- Genetic predisposition (certain gene mutations can control the activation of immune cells). Important: Genes can create susceptibility, but environment and daily habits dictate whether symptoms show up.
- Food triggers in a sensitized system (not just “bad foods” more like the threshold is low).
4) Motility problems (your gut traffic is off)
Motility goes off when the body is either:
- in defense mode (rush it out or clamp down), or
- out of rhythm (hormones, sleep, timing, hydration, movement). See how the rhythms run your health in order to understand the big picture.
Too fast: this is the “everything rushes through” pattern (urgency, diarrhea, cramping).
- High stress / fight-or-flight mode (your body prioritizes escape, not digestion)
- Infections or food poisoning (the body speeds exit as a defense)
- Inflammation in the gut (including IBD flares)
- Stimulants (a lot of caffeine for some people)
- Certain foods that pull water in (some sugar alcohols, high-FODMAP loads for sensitive people)
- Hormone shifts (cycle, pregnancy, thyroid)
Too slow: this is the “stuck / backed up” pattern (constipation, bloating, heaviness).
- Pelvic floor coordination issues (you can have the urge but can’t fully empty)
- Low thyroid function patterns (slower overall pace)
- Higher progesterone states (common in the luteal phase and pregnancy)
- Chronic stress (for many people stress slows motility and tightens the gut)
- Dehydration + low electrolytes
- Low fiber or sudden fiber increase (either extreme can slow things depending on the person)
- Low movement / sedentary days
- Medications (common culprits include some pain meds, anticholinergics; varies)
5) Elimination isn’t smooth
In a “smooth elimination” pattern, you can go to the bathroom regularly, without straining, and you feel done afterward.
Elimination problems usually come from one (or a mix) of a few root causes. Think of it like a drain that isn’t clearing well: it can be too little water, slow pipes, tight valves, or poor timing/signals.
When elimination isn’t smooth, it often looks like:
- constipation (hard stools, skipping days)
- straining or needing a long time on the toilet
- feeling incomplete emptying (you still feel “full” or backed up)
- stools that are dry, small, or hard to pass
- or the opposite: stools that are loose and urgent (too fast to form well)
A quick way to guess what’s driving it:
- Hard/dry stools and pellet-like – usually not enough hydration + sat in the colon too long (things are moving slowly).
- Soft stools but hard to evacuate – more about the exit mechanics, the muscles aren’t relaxing and coordinating well, so it’s hard to pass even soft stool.
- If constipation comes with big bloating and keeps changing (better, worse, back again) – that pattern often points to a mix of sluggish/irregular movement plus extra fermentation (gas production), often made louder by stress and nervous system tension.
Now the part most people miss: digestion is run by more than “Body”
This is where my 3-layer framework makes digestion easier to understand.
1) BODY: the physical digestion system
This includes:
- stomach acid, enzymes, bile
- the absorption surface (your “carpet”)
- the microbiome
- motility (how fast things move)
- elimination
When Body is stressed, you see classic symptoms: reflux, bloating, gas, constipation, diarrhea, nutrient deficiencies and food sensitivities.
2) MIND: the nervous system (gut–brain axis)
Your gut and brain talk constantly. If your system is in fight-or-flight, digestion changes, sometimes dramatically. In “emergency mode,” the body does not prioritize deep digestion.
Mind includes:
- stress response and nervous system tone (how you perceive stress and how efficiently you switch between active and restful states)
- pain sensitivity (people with functional GI disorders perceive pain more acutely, their brains are more responsive to pain signals from the GI tract. Stress can make the existing pain seem even worse).
- negative thinking paterns (rumination, worry, hypervigilance)
- emotional patterns like using food for comfort or control
3) ENERGY: your overall state (safe vs braced)
This is the layer people feel but don’t always have language for.
Energy includes:
- whether you feel at ease/fulfilled or on guard/reserved
- whether your body feels safe enough to soften or tense and rigid
- whether you feel connected and supported / or isolated, lonely and tense
Call it nervous system “weather.” When your inner weather is stormy, your gut often becomes more reactive.
These three layers always affect each other
So symptoms are rarely caused by one thing. More often, one layer starts the loop and the others join in. And most often (but not always) all starts at the energy level (the overal feeling about your life or situation dictates your emotions and actions), and you see the result at the end, in the pshysical body, through pain and discomfort.
What typically starts digestive dysregulation
Digestive dysregulation usually starts when the gut’s inputs, timing, or immune environment change: sometimes suddenly (a bug, antibiotics, stress), sometimes gradually (chronic stress, diet patterns, hormone shifts). Most of the time it’s one (or a few) of these starters:
1) A trigger event (the classic “before and after”)
- a major stressful life period/event (accompanied by poor sleep)
- stomach bug / food poisoning / chemical exposure (pollutants)/ acute illness
- a round (or several rounds) of antibiotics
- travel + different food/water + disrupted routine
- pregnancy/postpartum/ motherhood
- frequent use of medication (common ones include NSAIDs, some antidepressants, iron, blood pressure medications, anti-acids etc.)
These can disrupt motility, microbes, inflammation, or barrier function quickly.
2) Chronic stress + low recovery (slow burn)
This is one of the most common modern patterns:
- stress stays chronically high
- sleep is lighter and iregular
- meals are low quality, processed, rushed or irregular
- the nervous system lives in “on” mode most of the time
Over time that can lower digestive output (breakdown), disrupt motility, and keep the gut more reactive.
3) Diet pattern changes (inputs the gut can’t handle well)
Not “one food,” but patterns like:
- lots of ultra-processed foods and additives (for some people)
- low fiber + low plant diversity (microbiome narrows)
- sudden high fiber/raw foods when the gut is already sensitive and inflammmed
- frequent snacking/no meal rhythm (motility and secretions lose timing)
- alcohol, excess caffeine, low hydration
If you want a simple next step, use my guide to build a healthy balanced plate.
4) Immune-driven conditions (defense system overactivation)
Sometimes the starter isn’t lifestyle at all:
- celiac disease (gluten-triggered autoimmunity in susceptible people)
- IBD (immune inflammation in the gut)
- true food allergy
In these cases, food and stress can amplify symptoms, but the underlying driver is immune activity.
5) Hormone/metabolic shifts (timing changes)
Hormones directly affect gut movement and sensitivity:
- thyroid changes (slower or faster motility)
- cortisol rhythm disruption (stress/sleep)
- hormonal changes (pregnancy/postpartum/perimenopause/ long-term use of combined hormonal contraceptives/ use of products that disrupt hormones, like plastic and pesticides)
- blood sugar swings
6) “Threshold” buildup (realistic explanation for many people)
Often it’s not one cause, it’s stacking: stress + poor sleep + rushed / nutritionally deficient meals + sugar swings + antibiotics history +use of toxic household products + sensitivities …and for some people even mold exposure….. then one extra stressor, pushes the system past its coping point.
A common modern pattern, is often observed as a slow drift, not a sudden breakdown:
Life is busy, stress stays high constantly, and the body doesn’t get many chances of true downtime and time off. People eat on the go, chew less, snack more, rely on coffee and low quality food (because is tasty / addictive), and sleep isn’t deep enough to reset the system. Digestion starts running “half-on,” so food isn’t broken down as well, the gut moves too slow or too fast, and bloating becomes normal.
Then one extra stressor – an illness, antibiotics, travel, exposure to chemicals that disrupt hormones, a hard life period – pushes the system past its limit, and what used to be mild discomfort turns into noticeable sensitivities and regular symptoms.
The most useful “sorting tool”: what’s loudest right now?
Most people aren’t dealing with one single cause. They’re dealing with a few overlapping drivers, but usually one is the main “volume knob” at the moment. When you can identify what’s running the show right now, everything becomes easier to navigate.
Here are simple signals:
When it’s mostly food-based
- symptoms are predictable and repeatable after specific foods
- timing is consistent (you can almost “set a clock” by it)
- removing the trigger food brings noticeable relief
When it’s mostly nervous system-based
- symptoms change with stress/safety, travel, pressure, conflict, or poor sleep
- appetite changes (significant loss of appetite or overeating) after a stressful event
- you react to “safe foods” during stressful times
- your gut feels calmer when life feels calmer
- tests for physical, structural damage come back negative.
When it’s mostly hormone-based
- symptoms shift with cycle (PMS week, ovulation), pregnancy, postpartum, perimenopause
- sleep loss strongly worsens digestion
- thyroid/blood sugar imbalances (weight changes, mood fluctuations, skin and hair changes)
- heartburn, constipation/bloating or looser stools show up in repeat phases (abnormal abdominal distension, despite having a normal weight)
- digestive symptoms persist despite diet changes, high fiber, and medication.
When it’s mostly immune-based + inflammation
Approximately 70-80% of our immune system resides in the gut. One of the primary element linking gut health to autoimmune diseases is increased intestinal permeability, aka “leaky gut syndrome”.
If you have a compromised intestinal barrier (it fails to act as a tight, selective barrier) combined with an imbalaned gut microbiome (meaning more “bad” bacteria than “good”) plus you’re genetically susceptible, you can say that the probability that you opened the door for the development of an autoimmune disease is very high.
This combination allows for a cascade of events where the immune system is mis-directed, leading to chronic inflammation and, in genetically susceptible individuals, the initiation of self-tissue attacks.
Individuals with autoimmune conditions often exhibit these patterns:
- flares last longer than a single meal. They last days/weeks and feel more “inflammatory”.
- your tolerance drops overall (it’s not one food, it’s that everything feels harder to handle).
- systemic signs (anemia, vitamin B deficiency, fatigue that feels heavy, chronic brain fog, achy joints and general stiffness, muscle weakness, skin rashes (usually dry), mouth sores, geographic tongue, low-grade fever).
- “flare” pattern: symptoms often come and go, with periods of high activity (“flares”) and remission.
- difficult to diagnose: because symptoms can mimic other illnesses, diagnosing requires a detailed history, blood tests (such as ANA), and examination by a specialist.
Note: gut permeability is often a long-term consequence of something else (IBD, celiac, infection, chronic stress, microbiome disruption), not usually a stand-alone diagnosis.
If inflammation is part of your pattern, this anti-inflammatory foods guide can help you simplify your next food choices.
Red-flag reminder: if you have blood in stool, unexplained weight loss, fever, anemia/iron deficiency, persistent diarrhea (especially waking you at night), or severe pain, get medical evaluation.
When it’s energy/state-based (more than “mental health”)
This is a little different than the nervous system category. Nervous system is often about obvious stressors. Energy/state is about the deeper tone underneath, whether your system feels open and at ease or braced and guarded, even when life looks “fine” on paper.
Clues it’s more energy-based:
- you’re not necessarily anxious, but you feel subtly tense, heavy, or on guard most of the time
- symptoms flare in certain people/places/environments even without obvious stress (a room feels “tight,” a conversation drains you, your body contracts)
- your digestion shifts with connection vs isolation (you digest better when you feel supported, seen, or safe. And worse when you feel alone, pressured, or emotionally shut down)
- you notice gut symptoms after emotional suppression (holding back tears/anger, people-pleasing, “powering through”) more than after a stressful event.
- regulation happens fastest through state-shifters: music, nature, sunlight, prayer/meditation, breath + rhythm, gentle movement. Things that change your felt sense, not just your thoughts
Example: You’ve eaten the same “safe” breakfast all week. On a day you feel grounded and connected, it digests fine. On a day you feel tense, worried or fearful (even without a clear reason), you bloat or get tight in your stomach or you get an auto-immune flare-up. Nothing changed in the food, but the state did.
And yes, most people are mixed:
A fear or worry about life in general (silent in the backgroynd) + stressful week + poor sleep + menstrual cycle shift + trigger food can create a “perfect storm.”
The goal isn’t to label yourself, it’s to notice which driver is loudest so you know where to focus first.
The cascade: how Body, Mind, and Energy affect each other
Here’s another way to see the cascade: digestion has hardware and software.
- Hardware – the gut’s parts and tissues (lining, immune activity, microbiome, enzymes, inflammation).
- Software – the signals that tell the hardware how to run (nervous system: safety vs threat, emotional state, thinking patterns, energy state – the felt sense of ease / fulfillment or alert / danger).
When software is stuck in “threat,” the hardware shifts into protection mode: less acid and enzymes, altered motility, more sensitivity, and a more reactive immune system.
When software returns to “safe enough,” the hardware has a better chance to do its job: break down food, absorb, repair, and calm inflammation over time.
Think of digestion as a system that’s always asking one question:
“Is it safe to digest and repair right now?”
When the answer is yes, the body can break down food, absorb nutrients, move things along, and eliminate waste smoothly.
When the answer is no (or the body thinks it’s no), digestion becomes a lower priority, and the system shifts into protection/surviving mode.
A simple chain reaction (most common)
- Energy/state shifts first. You feel unfulfilled, discouraged, frustrated, guarded, disconnected, or “on edge,” sometimes without a clear reason…. or with a valid reason and you feel powerless.
- That state becomes nervous system tone (mind senses “not safe”). The body leans more toward fight-or-flight (sympathetic nervous system activation): muscles and fascia tighten (first sign), breath shortens, blood flow shifts away from digestion and it runs “half on.”
- Then the Body layer follows:
- less digestive output (acid/enzymes/bile timing can drop)
- motility changes (too fast or too slow)
- gut becomes more sensitive and reactive (pain signals get louder)
- The gut starts sending signals back up: discomfort, bloating, urgency, fatigue – then your brain interprets that as more threat which increases vigilance/anxiety and tightens the stress loop.
That’s the feedback loop: state > signals > symptoms > more state.

Create the Conditions for Repair
You can remove every obvious trigger and still feel stuck if your system is living in “threat mode“. That’s because digestion and healing don’t happen best when the body is tense and braced. They happen when the body gets enough signals of safety to switch into rest-and-digest (parasympathetic mode).
This is where “software support” matters.
Regulation practices help the system shift out of threat so repair can actually happen (software support). Not because your symptoms are “in your head,” but because the nervous system controls the volume of digestion: saliva, stomach acid, enzyme release, motility timing, inflammation signals, and even how strongly you feel gut sensations.
In real life, this means your goal isn’t only perfect food, it’s a more regulated baseline. When the system is calmer, you get less bloating, less urgency, and fewer flare-ups. And over time, that calmer state makes it easier for the body to rebuild the gut lining, stabilize the microbiome, and lower unnecessary immune reactivity, while you also address the true “hardware” pieces (like specific triggers, deficiencies, infections, or diagnosed conditions).
Regulation practices that help digestion “turn on”
These aren’t complicated. The goal is to send your body the message: “I’m safe enough to digest.”
- Slow down before meals (60–90 seconds): slow exhale breathing, hand on belly, unclench jaw/shoulders.
- Eat slower + chew more: not perfect, just less rushed.
- Meal rhythm: fewer random snacks, more consistent meals, earlier dinners when possible.
- Post-meal gentle movement: a 5–10 minute walk helps motility and reduces stress chemistry.
- Light + sleep basics: consistent bedtime, reduce late-night stimulation and expose yourself to morning daylight.
- Nervous system support during the day: music, nature, prayer/meditation, humming/singing, dancing, jumping, socializing, breathwork, tapping technique (EFT) anything that reliably softens you.
- Emotional expression: journaling, naming feelings, letting your body discharge tension (shake out arms/legs, stretch, a good cry, talk with a friend).
- Reduce threat around food: simplify meals, avoid constant tracking/testing, take breaks from doom-scrolling health info.
- Build safety in the body (somatic basics): slow breathing + longer exhales, gentle rocking, supported rest, warmth on the belly.
Pick 1–2 practices and repeat them daily, then add more. Consistency trains your nervous system faster than doing 10 things once.
Where You Can Start
You don’t need to fix everything at once. Start where the pattern is loudest right now:
If it’s mostly food/chemistry-based: Start with the simplest repeatable change. remove the clear trigger(s) and simplify meals for a short window, then re-test calmly. Focus on consistency more than perfection.
If it’s mostly nervous-system based (stress physiology): Start by regulating around meals and sleep. Use the regulation practices mentioned above.
If it’s mostly hormone/metabolism-based: Start with rhythm. Dteady meals (especially protein), morning light, and more consistent sleep. Track symptoms against your cycle and sleep, patterns usually show up fast.
If it’s mostly immune/inflammation-based: Start with getting clarity and reducing obvious triggers while supporting your baseline (sleep, nourishment, stress load). If symptoms are persistent or intense, prioritize proper medical evaluation. A functional medicine doctor can guide you.
If it’s mostly energy/state-based: Start with what shifts your felt sense of safety: nature, music, prayer or meditation, breath + rhythm, gentle movement, or supportive human connection. Your goal is “less bracing” in the body, less thinking and more doing and being.
If you found this information helpful, don’t hesitate to comment below and join my newsletter. I’ll be coming up with more in the future.
New here? Start with my “Getting Started” page for the simplest basic steps. Or explore more below.
Explore More
©HealthyTasteOfLife. Content and photographs are copyright protected and need prior permission to use. Copying and/or pasting full recipes to other websites and any social media is strictly prohibited. Sharing and using the link of this recipe or article is both encouraged and appreciated!